About Lung Health, Lung Failure, Lung Disease, Lung Conditions, Disease Causes, Symptoms & Treatment
Today's date of is a good time to start thinking about ways to stop or even reverse Lung Failure - below are conditions which may cause lung disease and lung failure:
- Drug-induced pulmonary disease is a cause of lung failure.
- Drug-induced pulmonary disease is lung disease brought on by a bad reaction to a medication.
Causes of Lung Failure and Lung Disease
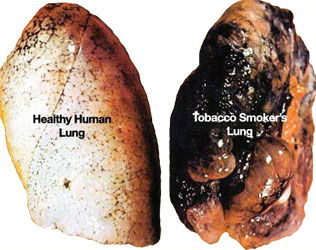
Not too surprisingly, the most serious cause of lung failure, lung disease, lung cancer, Emphysema and COPD is little doubt from smoking. With that said; if you smoke PLEASE STOP NOW!
However, some types of lung damage may result from medications, and (contrary to smokers) it's typically impossible to predict who will develop lung disease resulting from meds or drugs.
The types of lung diseases that may result from medications include:
- Allergic reactions -- asthma, hypersensitivity pneumonitis, or eosinophilic pneumonia
- Alveolar hemorrhage, which is bleeding into the lung air sacks
- Bronchitis
- Drug-induced lupus erythematosus
- Granulomatous lung disease -- a type of tumor in the lungs
- Inflammation of the lung air sacks (pneumonitis or infiltration)
- Interstitial fibrosis
- Lung failure
- Lung vasculitis, which is inflammation of lung blood vessels
- Mediastinitis
- Pulmonary edema
- Pleural effusion
- Swollen lymph nodes
Many drugs are known to cause lung disease in some people, including those used during chemotherapy and to treat certain heart conditions. Other drugs known to cause lung disease in some people include certain antibiotics and illicit drugs.
Symptoms of Lung Failure
- Bloody sputum
- Chest pain
- Cough
- Fever
- Shortness of breath
- Wheezing
Note: Symptoms may vary from person to person.
Exams and Tests of Lung Failure
The doctor will perform a physical exam and listen to your chest and lungs with a stethoscope. Abnormal breath sounds may be heard.
Tests that may be done include:
- Bronchoscopy
- Complete blood count with blood differential
- Chest CT scan
- Chest X-ray
- Lung biopsy (in rare cases)
- Thoracentesis (if pleural effusion is present)
Treatment of Lung Failure
The first step is to stop using the prescription drug causing the problem. Other treatments depend on your specific symptoms. For instance, you may need oxygen until the drug-induced lung disease improves. Powerful anti-inflammatory medicines called steroids are sometimes used and may quickly reverse the lung inflammation.
Outlook / Prognosis of Lung Failure
Acute episodes usually go away within 48 - 72 hours after the medication has been discontinued, but chronic syndromes may take longer to resolve. Some drug-induced lung diseases such as pulmonary fibrosis may never go away.
Possible Complications of Lung Failure
Diffuse interstitial pulmonary fibrosis
Hypoxemia (low blood oxygen)
Respiratory failure
When to Contact a Medical Professional
Call your health care provider if you develop symptoms of this disorder.
Prevention of Lung Failure
Any previous reaction to a medication should be noted, so that you can avoid the medication in the future. Wear a medical allergy bracelet if you have known drug reactions. Avoid the abuse of illicit drugs, as this will prevent many drug-induced lung diseases.
Pleural Effusion is a cause of Lung Failure
A pleural effusion is an accumulation of fluid between the layers of tissue that line the lungs and chest cavity.
Your body produces pleural fluid in small amounts to lubricate the surfaces of the pleura, the thin tissue that lines the chest cavity and surrounds the lungs. A pleural effusion is an abnormal, excessive collection of this fluid.
Two different types of effusions can develop:
- Transudative pleural effusions are caused by fluid leaking into
the pleural space. This is caused by elevated pressure in, or
low protein content in, the blood vessels. Congestive heart failure
is the most common cause.
- Exudative effusions usually result from leaky blood vessels caused by inflammation (irritation and swelling) of the pleura. This is often caused by lung disease. Examples include lung cancer, lung infections such as tuberculosis and pneumonia, drug reactions, and asbestosis.
Symptoms of Pleural Effusion
- Chest pain, usually a sharp pain that is worse with cough or deep breaths
- Cough
- Fever
- Hiccups
- Rapid breathing
- Shortness of breath
- Sometimes there are no symptoms
Exams and Tests for Pleural Effusion
During a physical examination, the doctor will listen to the sound of your breathing with a stethoscope and may tap on your chest to listen for dullness.
The following tests may help to confirm a diagnosis:
- Chest x-ray
- Pleural fluid analysis (examining the fluid under a microscope to look for bacteria, amount of protein, and presence of cancerous cells)
- Thoracentesis (a sample of fluid is removed with a needle inserted between the ribs)
- Thoracic CT
- Ultrasound of the chest
Treatment of Pleural Effusion
Treatment may be directed at removing the fluid, preventing it from accumulating again, or addressing the underlying cause of the fluid buildup.
Therapeutic thoracentesis may be done if the fluid collection is large and causing pressure, shortness of breath, or other breathing problems, such as low oxygen levels. Removing the fluid allows the lung to expand, making breathing easier. Treating the underlying cause of the effusion then becomes the goal.
For example, pleural effusions caused by congestive heart failure are treated with diuretics (water pills) and other medications that treat heart failure. Pleural effusions caused by infection are treated with appropriate antibiotics. In people with cancer or infections, the effusion is often treated by using a chest tube for several days to drain the fluid. Chemotherapy, radiation therapy, surgery, or instilling medication into the chest that prevents re-accumulation of fluid after drainage may be used in some cases.
Outlook/Prognosis of Pleural Effusion
The expected outcome depends upon the underlying disease.
Possible Complications
A lung surrounded by excess fluid for a long time may collapse.
Pleural fluid that becomes infected may turn into an abscess, called
an empyema, which requires prolonged drainage with a chest tube
placed into the fluid.
Pneumothorax (air within the chest cavity) can be a complication of the thoracentesis procedure.
When to Contact a Medical Professional
Call your health care provider if you have symptoms of pleural effusion.
Call your provider or go to the emergency room if shortness of breath or difficulty breathing occurs immediately after thoracentesis.