Body Dysmorphic Disorder (BDD)
People who have Body Dysmorphic Disorder (BDD) are constantly obsessing there is something wrong with their body, how they look or their body appears, even though the perceived appearance and flaw is in reality almost always minimal or even non-existent.
They may describe themselves as looking unattractive, fat, unusual, hideous, deformed, or ugly in appearance.  Those perceptions and concerns most often focus on the face or head (i.e., skin and skin color, acne, hair, skin defects, facial wrinkles, pimples, balding, eyebrows, teeth, ears, nose or even head size) but can include any other body area, or the entire body, with great over-concern about other body areas such as breast size and shape, buttocks and sagging skin body tightening, for example.
Those perceptions and concerns most often focus on the face or head (i.e., skin and skin color, acne, hair, skin defects, facial wrinkles, pimples, balding, eyebrows, teeth, ears, nose or even head size) but can include any other body area, or the entire body, with great over-concern about other body areas such as breast size and shape, buttocks and sagging skin body tightening, for example.
The appearance pre-occupations are difficult to resist or control, and on average consume 3 to 8 hours a day, such as looking in the mirror, for example.  They are often associated with fears of rejection and feelings of low self-esteem, shame, embarrassment, unworthiness, and being unlovable. Insight is usually poor, and nearly half of patients are delusional involving dysmorphic disorder, i.e., completely certain they look abnormal and their view of the 'defect' is indeed accurate.
They are often associated with fears of rejection and feelings of low self-esteem, shame, embarrassment, unworthiness, and being unlovable. Insight is usually poor, and nearly half of patients are delusional involving dysmorphic disorder, i.e., completely certain they look abnormal and their view of the 'defect' is indeed accurate.
A majority of "body dysmorphic disorder" sufferers have ideas or delusions of others noticing their alleged appearance defects, thinking other people are taking special notice of the believed 'defect', perhaps staring at it, talking about it, or mocking it behind their back, which very rarely actually happens (since the believed defects are far from being real or noticeable by others, in most all cases).
A good example of dysmorphophobia is a female who is actually 15-pounds under-weight but strangely believes she is over-weight and fat, so she is constantly dieting, fasting, going on an unusual or liquid diet, or even gets unnecessary colon cleansing (desiring to clean out her system) even though there is absolutely nothing wrong with her, she looks healthy and well, and really has normal or below normal body weight.
Most "body dysmorphic disorder" patients perform repetitive, compulsive behaviors aimed at examining, improving, or hiding the (wrongly) believed
'defect', including often seeking unnecessary cosmetic surgery, such as the woman in the picture
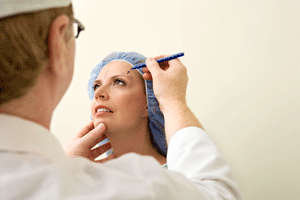 being examined by her physician for cosmetic plastic surgery, for an inconsequential and barely noticeable imperfection.
being examined by her physician for cosmetic plastic surgery, for an inconsequential and barely noticeable imperfection.
Typical behavior include mirror checking, comparing with others, not wanting their picture taken, reluctance to be seen in public (especially when dressed casually), excessive grooming (i.e., too frequent manicures, pedicures and beauty salon visits, applying makeup excessively, hair styling and hair dying), camouflaging (i.e., with a hat, clothing, or makeup), frequent clothes changing, reassurance seeking, skin picking, and eating a very unusual or highly restricted diet. These BDD and BDS behaviors typically occur for many hours a day and are difficult to resist or control. Some studies report an approximately equal gender ratio, whereas other research indicates a preponderance of women with this serious mental health condition.
A majority of patients have never been married, and a relatively high proportion are unemployed. The disorder's clinical features appear generally similar in women and men, although several differences are apparent. Body dysmorphic syndrome often begins during early adolescence and can occur in childhood. Although there is much research in this age group, body dysmorphic disorder's clinical features in children and adolescents appear similar to those in adults. Additional research and studies of body dysmorphic disorder's are needed since medical data indicates "body dysmorphic syndrome" is a chronic mental condition, often with waxing and waning symptoms. Most Body Dysmorphic Disorder patients seen in psychiatric settings also suffer from other mental disorders.
Research has discovered major depression is a most common issue, with a large medical study reporting a current depression rate of 59% and a lifetime rate of 79%. In this study, onset of major depression most often occurred after onset of Body Dysmorphic Disorder, consistent with clinical impressions that depression is often (although not always) secondary to Body Dysmorphic Disorder. Substance use disorders, social phobia, obsessive compulsive disorder and avoidance personality disorders also commonly co-occur with Body Dysmorphic Disorder.
Impairment in quality of life and level of functioning varies, Body Dysmorphic Disorder nearly always causes impaired functioning, often to a marked degree, as well as other complications. Social impairment is nearly universal. Individuals with Body Dysmorphic Disorder may have few or no friends, and may avoid dating and other social interactions. Most patients also have impaired academic, occupational, or role functioning. Body Dysmorphic Disorder obsessions, behaviors, or self-consciousness about being seen often diminish concentration and productivity. BDD patients not uncommonly drop out of school or stop working.
In one study, 30% had been completely house-bound for at least a week, more than half had been psychiatrically hospitalized, a majority have experienced suicidal ideas due to body dysmorphic disorder and dysmorphic syndrome, with some sufferers attempting suicide. Many people suffering from chronic body dysmorphic disorder can barely function, let alone enjoy a normal life. A study of acne dermatology patients who committed suicide reported most had Body and Acne Dysmorphic Disorder syndrome.
Body dysmorphic disorder patients also experience unusually high levels of real or perceived stress and an extremely poor quality of life. In a study assessing health related quality of life issues with a health survey, outpatients with Body Dysmorphic Disorder scored notably worse in all mental health domains vs normal numbers for the general US population and for patients with depression, type II diabetes, or a recent myocardial infarction. More severe Body Dysmorphic Disorder Symptoms were associated with poorer mental health-related quality of life.
BDD is a severe and relatively common psychiatric disorder that occurs around the world. However, it usually goes undiagnosed in clinical settings. It is important to diagnose BDD, as it causes significant impairment in functioning and is associated with markedly poor quality of life. SRIs and CBT are currently considered the treatments of choice. However, studies of all aspects of BDD are needed - in particular, treatment studies, epidemiology studies (in which BDD symptoms are specifically inquired about and differentiated from other common disorders such as hypochondriasis and OCD), cross-cultural studies, and investigation of BDD-related disability and the disorder's cost and burden to society.
Research is also needed on whether BDD may be more closely related to social phobia, OCD, or depression than to most of the other soma to form disorders with which it is classified.
To get health information about other disorders, disease and medical conditions please visit Wellness and Health Organization.




