Treatment of Superficial
Venous Reflux Disease
Today is which is a good date to get information for Venous Reflux Disease. Effective but at the same time also minimally invasive techniques for ablation of incompetent saphenous veins using either radio frequency or laser energy sources have gained acceptance and are being widely applied today. Tumescent local anesthesia provides protection to tissues surrounding the treated veins and allows the procedures to be done on conscious patients. Results thus far compare favorably with surgical stripping procedures.
Efficacy rates and complication rates support these techniques, and patient satisfaction appears high. Micro phlebectomy, also minimally invasive, has advantages over direct incisional excision of varicosities. Foam sclerosant injection therapy has been used extensively in Europe and is proving useful in treating refluxing pelvic veins and recurrent varicosities.
Over the past few decades lots of medical information has been learned about venous insufficiency, venous reflux disease and edema in the last few years new and exciting treatment options have been developed. These new methods of resolving venous hypertension in the superficial veins of the lower extremities are safe and offer better patient outcomes with significantly less patient inconvenience than prior surgical remedies.
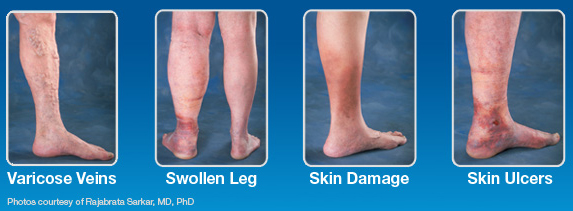
It's well established that superficial venous insufficiency (reflux) and its clinical presentation of varicose veins and related symptoms are the result of venous hypertension, which in turn is the result of failure of the venous valves. The complications of venous hypertension in addition to venous varicosities are chronic edema, hyper pigmentation, skin changes (lipodermatosclerosis), chronic ulceration, and variceal hemorrhage.
It's been estimated that more than 25 million people in the USA have superficial venous reflux in their legs, and perhaps 7 million exhibit serious complications such as chronic edema, skin changes, and ulceration. Perhaps in excess of 500,000 Americans suffer from debilitating chronic venous ulcers. Such ulcers are notoriously difficult to heal using usual wound management measures. It is generally accepted that many patients with varicose veins will go on to develop one or more of these complications if the venous hypertension is left untreated. Friedrich von Trendelenburg introduced modern surgical treatment of varicose veins in 1860 with an operation through a transverse incision in the upper thigh through which he ligated and divided the great saphenous vein.
 Charles Mayo, soon after graduating from medical school, began excising the great saphenous vein through a single incision from the groin to just below the knee. In 1906, he reported a series of 185 patients treated in this fashion. Mayo and Keller published separate descriptions of procedures using “stripping” devices each had devised early in the 20th century. Later, Thomas T. Myers of the Mayo Clinic published results using a flexible stripper for removal of the great saphenous vein and direct excision of the varicosities.
Charles Mayo, soon after graduating from medical school, began excising the great saphenous vein through a single incision from the groin to just below the knee. In 1906, he reported a series of 185 patients treated in this fashion. Mayo and Keller published separate descriptions of procedures using “stripping” devices each had devised early in the 20th century. Later, Thomas T. Myers of the Mayo Clinic published results using a flexible stripper for removal of the great saphenous vein and direct excision of the varicosities.
This popular vein-stripping operation was the treatment of choice from 1950 until recently; it has been widely applied and is still performed by many surgeons. The operation has major drawbacks, however: it requires general or spinal anesthesia; limits patients' activity and causes them to miss work; and is associated with a significant infection rate, a high incidence of postoperative paresthesias and pain, and a high incidence of recurrent varicosities, which has been reported to be as high as 70% at 10 years.
Fortunately today varicose veins can be treated with new and promising treatment modalities. These include venous ablation procedures using radio frequency, laser, and foam sclerotherapy. While these procedures have been available only in the last few years, a growing body of data supports their effectiveness.
Endovenous laser ablation of the great saphenous vein. Merchant et al reported the results of radio frequency ablation of truncal veins in 1222 limbs. Vein occlusion as evaluated by ultrasound duplex scanning was 96.8% at 1 week and 87% at 1 and 5 years. Absence of reflux in the limb was 96.6% at 1 week and decreased to 88% and 83.8% at 1 and 5 years, respectively. The late reappearance of venous reflux was attributed to missed refluxing veins at earlier examinations or the development of reflux in veins that appeared normal at the time of treatment. Complications included deep vein thrombosis, 0.9%; skin burns, 1.2%; clinical phlebitis, 2.9%; infection, 0.2%; and paresthesias, 12.3%. In a recent review of published clinical series, the incidence of thrombus extension into the common femoral vein or deep vein thrombosis was 2.1% after radio frequency ablation and 0.3% after laser ablation.
When evaluating the results of endovenous ablation of truncal veins, it is necessary to consider the wavelength of the laser. Min and Khilnani reported the results in 499 limbs treated with the 810-nm diode laser. Vein occlusion was documented in 98% of limbs at 1 week and in 93% of limbs at 2 years. There were no instances of deep vein thrombosis, skin burns, or paresthesias. Increased bruising was noted in 24% of limbs. In a series of 452 limbs treated with the 1320-nm laser, vein closure occurred in 98.6% at both 6 months and 1 year (J. R. Kingsley, personal communication, 2006). It is necessary to compare results of the minimally invasive endovenous ablation procedures using either radio frequency or laser against the results of the vein-stripping surgical procedure. Multiple series of vein-stripping patients have demonstrated significant recurrence rates of 15% to 70% over the course of 5 to 10 years.
Patient satisfaction with the vein-stripping procedure has been disappointing, with only 85% of patients rating the results excellent or good. This comparison does not take into account the increased pain and morbidity, the requirements for general or spinal anesthesia and hospitalization and the resulting expense, and the physical limitations and absence from work following the stripping operation. It is important to note that long-term follow-up of patients undergoing radio frequency or laser venous ablation is limited.
FOAM CHEMICAL ABLATION
Foam sclerotherapy was developed in Europe and has gained popularity over the past few years. Using Tessari's method, the sclerosant solution is mixed forcefully with air or carbon dioxide using a technique employing two syringes and a three-way connector to create a foam, which is injected directly in the veins being treated. The sclerosant, which coats the gas bubbles, tends to linger against the endothelial surface of the veins rather than be washed out. This allows more contact time for the sclerosant to cause endothelial and vein wall damage by interfering with the function of endothelial and subendothelial cell surface proteins that are necessary for cell survival.
The end result is thrombosis and fibrous obliteration of the vein. Cabrera has used foam sclerotherapy as a single therapy to ablate truncal veins such as the great saphenous vein. Others have used foam in conjunction with radio frequency to achieve results superior to either alone. Morrison reported 1445 great saphenous veins treated with radio frequency.
At a mean follow-up of 27 months, success, as measured by sonographic absence of the great saphenous vein, occurred in <50% of the limbs. Of the veins with persistent flow, 80% were successfully closed with ultrasound-guided foam sclerotherapy. However, with the combination of radio frequency and foam sclerotherapy, he achieved 94% closure (N. Morrison, personal communication, 2006). Adverse events are rare, but reported symptoms following foam injection include visual disturbance, cough, and migraine, all of which are transient and usually clear within minutes.
Clearly, foam chemical ablation has been a useful tool in treating recurrent veins after treatment with endovenous ablation methods. It has also been successful in treating varicosities emanating from pelvic venous reflux, which produces vulvar, high thigh, and posterior thigh painful varicosities. It is the best method of ablating incompetent communicating veins and perforators. These veins, which perforate the fascia generalis overlying the muscles of the leg, carry venous flow and transmit high pressure from the deep veins of the muscles into the superficial veins of the leg.
SUBFASCIAL ENDOSCOPIC PERFORATOR VEIN SURGERY
With the popularity of minimally invasive endoscopic surgery, surgeons began to apply the technique to interrupt incompetent perforator veins in the sub fascial space. The sub fascial endoscopic perforator vein surgery (SEPS) approach avoided the larger and in many cases multiple incisions necessary to divide the communicating veins, as described by Linton. The SEPS operation has been shown to be effective in accelerating ulcer healing and in preventing recurrences. It has the disadvantage of requiring general or spinal anesthesia, and patients experience some wound pain and disability for a while. It appears that foam chemical ablation using a sclerosant is less invasive and safely accomplishes perforator closure without incisions and division of the vessels.
MICROPHLEBECTOMY
In the past, incisions have been used to excise bulging superficial varices, which typically course in the fat layer above the muscle fascia and below the skin. These unsightly and painful veins are removed for cosmetic reasons and to prevent superficial thrombophlebitis that often occurs in these varicosities once the venous hypertension has been alleviated by one of the techniques described above. By removing the varicosities, skin hyper pigmentation is also avoided should clotting of the varicosities occur. Large incisions have been effective but leave significant scars.
Micro phlebectomy, which was described by Muller and is often referred to as ambulatory phlebectomy, allows the removal of the varicosities quite effectively without leaving objectionable scars. Tiny 2- to 3-mm incisions are made over the bulging varicosities, which have been marked with the patient in a standing position. Through these incisions, a small vein hook delivers the varicose vein, which is clamped, teased out, and excised. Micro phlebectomy has proven to be a very esthetic method of removing the varicosities and is easily accomplished using tumescent local anesthesia.
Micro phlebectomy of superficial venous varicosity. The vein is (a) hooked through a tiny incision and (b) clamped, teased out, and excised. CONCLUSIONS. Most patients require a combination of treatment methods depending on the point of highest venous reflux, the presence of bulging varicosities, the presence of incompetent perforator veins, and the depth of subcutaneous tissue overlying the muscle fascia. Radio frequency or laser ablation in combination with micro phlebectomy and foam sclerotherapy has been shown to achieve excellent clinical and cosmetic outcomes.
Thanks to new developments in endovenous ablation, the treatment of venous reflux disease of lower extremities may be performed as a minimally invasive procedure under local anesthesia in an outpatient setting. Patients return to usual activities in 1 or 2 days. Recurrence rates are acceptably low, and if a recurrence should occur, early treatment with foam chemical ablation is easy and effective. Overall patient satisfaction with these modern techniques surpasses that with the vein-stripping operation of the past.




