Deep Skin Wrinkles Skin Care Treatment Guide
"Deep Skin Wrinkles" your deep-wrinkles treatment source... on a mission of providing Deep Skin Wrinkles information and skin beauty options to eliminate or reduce appearance of ugly wrinkles...
There are several ways to get rid of wrinkles.
A face lift is the most effective and long lasting procedure.
Botox® is another solution to getting rid of deep skin wrinkles by skin tightening. However Botox® injections need to be repeated and the deeper the wrinkles the more injections you need.
A chemical peel is another way to try and diminish deep skin wrinkles. A chemical peel can be harsh on the skin, since it's a chemical that causes the skin to peel, however it can be effective in removing wrinkles. This causes the skin to appear burned for several weeks. The skin will then flake off and new skin cells will grow for a less wrinkled appearance.
Face Lift
Sometimes the only way to effectively eliminate deep wrinkles is by cosmetic surgery. A face lift not only will get rid of wrinkles, it will also help skin sag giving you a more youthful appearance. A face lift is an extensive procedure that requires a level of commitment not necessary for other wrinkle treatments. A face lift is a surgical procedure. During the face lift procedure, the doctor literally lifts the skin off of the face, often removing excess skin, tightens up the tissue over the bone structure and then repositions the skin over the tissue. It often requires an overnight hospital stay because the face lift surgery takes several hours to complete.
Botox Injections
Another method that can be tried for wrinkles is Botox injections. 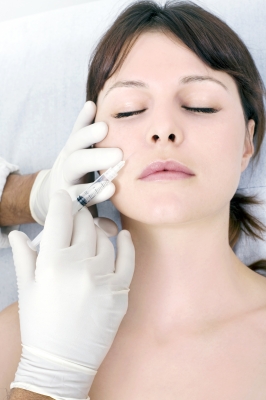 Botox injections are becoming very popular and both women/men are turning to Botox injections to get control of their wrinkles. A small amount of Botox is injected and causes the muscles to relax, this in turn causes the wrinkles to relax.
Botox injections are becoming very popular and both women/men are turning to Botox injections to get control of their wrinkles. A small amount of Botox is injected and causes the muscles to relax, this in turn causes the wrinkles to relax.
Chemical Peel for Deep Wrinkles
Since it's a known fact that deep wrinkles are much harder to get rid of or diminish. If using products with moisturizers that are known to fight wrinkles such as vitamin A and E, alpha hydroxyl, or natural ingredients such as grape seed oil haven’t begun to change your wrinkles, it's probably time to check into a more clinical method of removing deep wrinkles.
A chemical peel could diminish those deep wrinkles. A chemical peel can be harsh on the skin, since it's a chemical that causes the skin to peel, however it can be an effective method of removing wrinkles. With deep wrinkles, a longer chemical peel would be required. This means leaving the chemical on for a longer time before removing it. This will cause the skin to appear to be burned for several weeks and then the skin will flake off and new skin cells will grow for a less wrinkled appearance.
Chemical peeling is a popular, relatively inexpensive, and generally safe method for treatment of some skin disorders and to refresh and rejuvenate skin. Chemical peels are classified by the depth of action into superficial, medium, and deep peels. The depth of the peel is correlated with clinical changes, with the greatest change achieved by deep peels. However, the depth is also associated with longer healing times and the potential for complications.
A wide variety of peels are available, utilizing various topical agents and concentrations, including a recent salicylic acid derivative, β-lipohydroxy acid, which has properties that may expand the clinical use of peels.
Superficial peels, penetrating only the epidermis, can be used to enhance treatment for a variety of conditions, including acne, melasma, dyschromia, photo damage, and actinic keratoses.
Medium-depth peels, penetrating to the papillary dermis, may be used for dyschromia, multiple solar keratoses, superficial scars, and pigmentary disorders.
Deep peels, affecting reticular dermis, may be used for severe photo aging, deep wrinkles, or scars. Peels can be combined with other in-office facial resurfacing techniques to optimize outcomes and enhance patient satisfaction and allow clinicians to tailor the treatment to individual patient needs.
Currently, new laser techniques are a popular alternative for major deep skin resurfacing because they avoid the adverse effects of deep chemical peels, even if phenol is used in lower concentrations.
Successful outcomes are based on a careful patient selection as well as appropriate use of specific peeling agents. Used properly, the chemical peel has the potential to fill an important therapeutic need in the dermatologist's and plastic surgeon's armamentarium. Peels are best performed and/or supervised by dermatologists and plastic surgeons who have far more experience and knowledge with cosmetic procedures than other physicians.
Chemical peels are very common in clinical practice.
Chemical peels are a mainstay in the cosmetic practitioner's armamentarium because they can be used to treat some skin disorders and can provide an aesthetic benefit. In addition, chemical peels may be combined with other resurfacing including face resurfacing and other rejuvenation procedures, often providing synergistic treatment and more flexibility in customizing treatments to patient needs and conditions. Clinicians can customize regimens to the patient's individual needs using several modalities, such as at-home skin regimens, chemical peels, and lasers or dermabrasion, to provide unheralded flexibility in individualized care.
Potential Side Effects of Peels
Superficial peels are safe and tolerated with mild discomfort, such as transient burning, irritation, and erythema.
Scarring is rare in superficial peels, as are PIH and infection. In medium and deep peels, lines of demarcation that are technique related can occur. Care should be taken to feather peel solution at junctions with non peeled skin to avoid this effect. Side effects of deeper peels can also include pigmentary changes (e.g., PIH for dark-skinned individuals), infections, allergic reactions, improper healing, hypersensitivity, disease exacerbation, and those due to improper application.
Care must also be taken to prophylactically treat patients with a history of herpes viral infection. Herpetic episodes, usually on the lip or above the vermilion border, may be prevented with prophylactic oral acyclovir, valacyclovir hydrochloride, or famciclovir. Antiviral agents are especially useful in patients who indicate a strong history of multiple herpetic lesions each year.
The best way to prevent complications is to identify patients at risk and maintain an appropriate peel depth that balances efficacy with known adverse events. Patients at risk include those with PIH, keloid formation, heavy occupational sun exposure, a history of intolerability to sunscreens, and uncooperative patients.
Tolerability of peels may be influenced by many factors, such as peel agents, concentration, depth, skin type, and concomitant use of skin care products. PIH can be exacerbated by sun exposure, so it is important to educate patients and closely monitor their recovery phase. Sunscreens should be used continuously to limit PIH development. Epidermal PIH responds well to various treatments, while dermal PIH remains problematic. Pretreatment with bleaching agents before beginning therapy with peels decreases the appearance of PIH. Treatment options include hydroquinone or kojic acid or other tyrosinase inhibitors.
In medium and deep peels, a common location of scarring is on the lower part of the face, due perhaps to greater tissue movement or more aggressive treatment. Other rare causes of scarring include infections and premature peeling, making post-peel monitoring an essential component of management. Delayed healing and persistent redness are early warning signs, and treatment with topical antibiotics and potent topical corticosteroids should be initiated as soon as possible to minimize scarring. Resistant scars may be treated with dermabrasion or pulsed dye laser followed by silicone sheeting therapy.
Acneiform eruptions may occur during or after peeling, presenting as erythematous follicular papules. These eruptions respond to oral antibiotics used in acne treatment. Discontinuation of oily skin preparations is also recommended.
Milia usually appear 2 to 4 months after peels in up to 20 percent of patients undergoing medium and deep peels and may be treated with extraction or electro surgery.
Medium-depth peels are associated with most of the complications described above, though most can be managed successfully. Medium- and deep-depth peels should be used with great caution on skin types IV to VI. Toxicity, although rare, has been reported with resorcinol, SA, and phenol deep peels.
Medical History of Patient
Taking a complete history prior to peeling is critical. It can enhance aesthetic results by identifying any factors that may contribute to problems and provides an opportunity to discuss adherence issues necessary for successful management.
It is important to gain insight into patients' perceptions of wound healing and scar formation, as well as prior experience with resurfacing procedures or face-lift surgery. Current literature recommends waiting at least six months after discontinuing oral isotretinoin therapy before performing resurfacing procedures.
A current medication list should be obtained, and photosensitizing agents should be discontinued. Some dermatological conditions, including rosacea, seborrheic or atopic dermatitis, and psoriasis, may increase the risk for postoperative problems, such as disease exacerbation, excessive and/or prolonged erythema, hypersensitivity, or delayed healing. Prophylactic antiviral agents should be prescribed as required. Since sun protection after peeling is essential, discussion in relation to the patient's past habits and experience is important.
Pretreatment
Pretreatment can help to enhance outcomes and is often started 2 to 4 weeks prior to the peel and discontinued 3 to 5 days before the procedure. Topical retinoids or a pre peel solution can help to create a smooth stratum corneum to achieve a more even penetration of the peel. Topical retinoids may also speed healing. Humphreys et al reported that pretreatment with a topical retinoid resulted in more rapid and even frosting as well as a decrease in telangiectasias, which the authors postulated as being due to deeper penetration of TCA with retinoid pretreatment.
Before a chemical peel, hydroquinone may be used to reduce the likelihood of PIH in dark-skinned individuals. Discussing peel after-effects with patients before the peel is also important to aid comprehension of the peeling process.
Post peel, patients should use a broad-spectrum sunscreen on a daily basis and implement a gentle cleansing regimen with toner and peel serum as prescribed. Moisturizers may also be recommended.
Maintenance of a Chemical Peel
After a chemical peel, edema, erythema, and desquamation may occur for 1 to 3 days for superficial peels and 5 to 10 days for medium to deep peels. A cleansing agent may be used and antibacterial ointment applied especially for deep peels. Patients should be instructed to avoid peeling or scratching the affected skin and to use only simple moisturizers.
A long-term maintenance program will preserve the results of chemical peels in most patients. Patient participation and education is required, emphasizing the importance of sun protection and the use of appropriate skin care regimens that include cleansing, toning, exfoliation, and moisturizers. Patients need to have realistic expectations and understand that achieving benefits from peels requires repeated procedures.
If the peel regimen works well for the patient, clinicians should consider a maintenance protocol, which may be one peel per month for six months, then every three months thereafter depending on the need and the season. Topical retinoid maintenance therapy can also help maintain the skin rejuvenation results achieved with a chemical peel. It may be used alone on a daily or intermittent basis or in addition to 2 to 3 weekly light peels periodically. Maintenance regimens may also include products with combinations of kojic acid, hydroquinone, LHA, SA, GA, or ascorbic acid.
Importance of Tailoring Therapy
It is important to develop a peel program that is tailored to the individual needs of the patient. For example, a patient with visible photo damage who can tolerate social and work downtime may be treated with a 35% TCA peel while another patient may be better treated with a series of lighter peels to minimize downtime. In addition, patients who are treated with peels may also be interested in a variety of other treatments, such as botulinum toxin or fillers, to improve the signs of aging.
Popularity of Chemical Peels
Chemical peels remain popular for the treatment of some skin disorders and for aesthetic improvement. Peels have been studied and shown to be effective as treatment for a myriad of conditions including acne, superficial scarring, photo damage, and melasma. Patients who are willing to undergo continued treatment are likely to be the best candidates.
Newer molecules such as the LHA superficial peel provide unique characteristics including targeted action and should be studied further. Clinicians should remember that there can be excellent synergy between peels and other procedures. Chemical peels are most effectively used in combination with a topical, at-home regimen, which, depending on the condition, may include exfoliating or moisturizing products, bleaching agents, or retinoids. Using peels less frequently but on a continuing basis is beneficial to help keep improvement ongoing, especially for superficial peels.
Medium peels and deep peels are used more judiciously over time, but can address particularly difficult conditions effectively over the course of several treatments. Finally, it is important for patients to use a good skin sun block for skin protection to optimize results achieved from chemical peels.





